 The literature differs on the prevalence of complications post coronary artery bypass surgery (CABG). These complications include:
The literature differs on the prevalence of complications post coronary artery bypass surgery (CABG). These complications include:
- Wound infection and bleeding
- Reactions to anesthesia
- Fever
- Pain
- Stroke, myocardial infarction, or even death
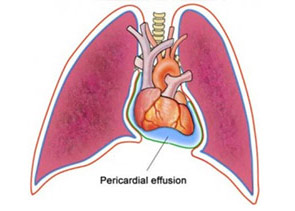
Some patients develop a fever associated with chest pain, irritability, and decreased appetite. This is due to inflammation involving the lung and heart sac. This complication sometimes is seen 1 to 6 weeks after surgeries that involve cutting through the pericardium (the outer covering of the heart). This reaction usually is mild. However, some patients may develop fluid buildup around the heart that requires treatment.
Memory loss and other changes, such as problems concentrating or thinking clearly, may occur in some people. These changes are more likely to occur in people who are older, who have high blood pressure or lung disease, or who drink excessive amounts of alcohol. These side effects often improve several months after surgery.
Use of the cardiopulmonary bypass machine increases the risks of blood clots forming in the blood. These can either go to the brain or block the flow of blood to the brain which may cause a stroke or other problems such as acute kidney injury.
In general, the risk of complications is higher if CABG is done in an emergency situation (for example, during a heart attack), if you’re older than 70, or if you have a history of smoking.
Your risk also is higher if you have other diseases or conditions, such as diabetes, kidney disease, lung disease, or peripheral arterial disease (Coronary Artery Bypass Grafting).
Today we will focus more closely on the risk of infection and bleeding into the pericardial sac (pericardial effusion).
Despite many recent improvements in intraoperative management and postoperative care, late pericardial effusions remain an important cause of morbidity after cardiac surgery. Pericardial effusions may delay recovery and can be life threatening when tamponade leads to hemodynamic compromise.
The Mayo Clinic did a study where they searched their patient database for the records of patients aged 18 years or older who underwent cardiac surgery with cardiopulmonary bypass at Mayo Clinic, Rochester, MN, from 1993 through 2005. Those who died on the day of operation were excluded. From this group they identified the study cohort, which consisted of patients in whom pericardial effusion developed within 30 postoperative days. Pericardial effusion was defined as fluid in the pericardial space that manifested with symptoms, required specific treatment, was large enough to prompt consideration of drainage, or required lengthened in-hospital stay for observation. Patients who did not meet the above criteria, required re-exploration for bleeding or tamponade within the first 3 days after surgery, or did not provide research authorization were excluded.
All other patients presumably did not have pericardial effusion after the operation and formed the first Control group (control 1).
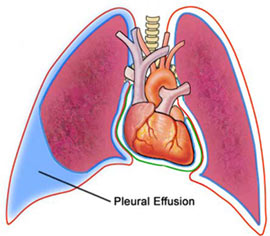
Pericardial effusion developed in 327 patients; these 327 form our study group and represent 1.5% of all patients undergoing cardiac surgery within the 13-year time frame. This incidence was 1.5% in 1993 through 1999 and 1.8% in 2000 through 2005. Pericardial effusion was commonly visualized by echocardiography at the end of the first postoperative week (mean [SD], 9 [6] days; median, 7 days). In 140 patients (43%) pericardial effusion was initially small, which progressed further to moderate or large in 81 patients (25%). Moderate or large pericardial effusion was usually seen approximately 2 weeks after the operation (13 [6] days). Pericardial effusions were associated with pleural effusions in 179 cases (55%); 104 bilateral, 65 left-sided, and 10 right-sided pleural effusions were seen on chest radiography. Also, 215 study patients (66%) had an enlarged cardiac silhouette.
Risk Factors for Pericardial Effusion
- Obesity
- Immunosuppression
- Pulmonary thromboembolism
- Renal failure
- Type of operation
- Prolonged cardiopulmonary bypass
The reported incidence of postoperative pericardial effusions ranges between 1% and 77%, depending on study definitions and designs. The higher incidences are reported from smaller prospective studies with frequent echocardiographic examinations; most of these effusions were clinically insignificant. In retrospective studies of clinically important pericardial effusions the reported incidence is 1% to 2%. In the current study, the incidence of observed pericardial effusion was relatively low (1.5%), probably because it was defined as fluid in the pericardial space that required intervention, lengthened in-hospital stay, or was large enough to prompt consideration of drainage. Therefore, cases of effusion that did not meet the above criteria or were not detected.
Conclusion
Several groups of patients are at increased risk for postoperative effusions. Patient care protocols, especially those concerning echocardiographic surveillance, should take these findings into consideration (Elena A. Ashikhmina, et al., 2010)
Works Cited
Coronary Artery Bypass Grafting. (n.d.). Retrieved October 28, 2013, from National Heart Lung and Blood Institute: http://www.nhlbi.nih.gov/health//dci/Diseases/cabg/cabg_all.html
Elena A. Ashikhmina, M., Schaff, MD, H. V., Sinak, MD, L. J., Dearani, MD, J. A., Suri, MD, R. M., Orszulak, MD, T. A., et al. (2010). Pericardial Effusion After Cardiac Surgery: Risk Factors, Patient Profiles, and Contemporary Management. Annals of Thoracic Surgery, pp. 112-118.
youtu.be
Where did you find the source for this?