 Untreated respiratory arrest and DEATH. Patient found asystolic with resulting DEATH. ST elevation goes unnoticed in a post anterior MI patient that had received a LAD stent. The patient infarcts, goes into v-fib and is unable to be resuscitated. These are all examples of what happens when monitor alarms are turned off, muted, or values are changed because the nurse gets tired of the ST elevation alarm going off (actual witnessed event that was thankfully corrected). Why do nurses turn off alarms, mute alarms, or change values? First I believe that in the cardiac patient, that is capable of going bad on a moment’s notice, the young nurse does not fully understand that these patients are truly time bombs waiting to go off. So forget for a moment that alarms are not meant to be turned off in the first place but in these instances I believe that lack of knowledge and experience plays into these types of actions.
Untreated respiratory arrest and DEATH. Patient found asystolic with resulting DEATH. ST elevation goes unnoticed in a post anterior MI patient that had received a LAD stent. The patient infarcts, goes into v-fib and is unable to be resuscitated. These are all examples of what happens when monitor alarms are turned off, muted, or values are changed because the nurse gets tired of the ST elevation alarm going off (actual witnessed event that was thankfully corrected). Why do nurses turn off alarms, mute alarms, or change values? First I believe that in the cardiac patient, that is capable of going bad on a moment’s notice, the young nurse does not fully understand that these patients are truly time bombs waiting to go off. So forget for a moment that alarms are not meant to be turned off in the first place but in these instances I believe that lack of knowledge and experience plays into these types of actions.
ALARM FATIGUE is a more prevalent reason for slow to no response to alarms. The Boston Globe enlisted the ECRI Institute, a nonprofit independent organization that researches the best approaches to safety, quality, and cost-effectiveness of patient care. They found 216 deaths nationwide from 2005-2010 that could be related to problems with monitor alarms. They also believe that this problem is under reported.[i]
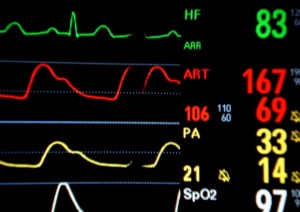
ICU monitors have the capacity to monitor not only heart rate but the different rhythms. The nurse can set the monitor to alarm for when the patient goes over a certain number of PVC’s in a minute; if the patient has PVC’s in couplets. The nurse can adjust the size of the ST segment that they are monitoring in the MI patients and CABG patients. Non-invasive and a-line blood pressure monitoring can be monitored. Turning off the a-line monitoring alarm can have lethal consequences if the a-line becomes disconnected. If this were to occur the patient may bleed out if not found in time. Swan-ganz catheters can be monitored also. This is important although many people do not use this alarm. If the swan balloon becomes permanently wedged the patient can go into v-fib and arrest. Your alarms should be set so that if this happens your alarms would go off to alert you; you would then notify the physician so that the Swan-ganz catheter could be repositioned. All monitors now monitor respirations and many alarm frequently if these leads are not placed properly.
Monitors have become much more complex and are capable of monitoring many more components Along with this advanced technology comes bell, whistles, beeps, and chirps. All of this creates an environment that overwhelms the ICU nurses senses and they become desensitized to the alarms. Eventually they can even tune out (not purposefully) even lethal alarms with the loudest volumes. This leads to slow response time to emergency events and again possible deaths.
Accuracy in setting alarms and in placing electrodes is extremely important to help in decreasing false alarm from being set off. Management in ICU’s should educate the staff regarding the importance of proper use of alarms and timely attention of alarms and explain that this is a national problem that needs attention. All staff should be educated on the proper use of the monitor in the ICU. Have the staff participate in developing a plan to decrease the inattention to monitor alarms thus making them feel part of the solution.
[i] Van Dam, Andrew, Alarm fatigue hurts patient care, overwhelms nurses “Association of Health Care Journalists
Feb. 17, 2011.
Leave a Comment