Legally where does the responsibility of the nurse begin and end? If an order that a physician writes causes harm to the patient and the nurse that followed through with the order had the knowledge and experience to know that the order could/would cause harm to the patient, does that nurse not bear some responsibility for the results of the order being followed? I believe in many instances that nurses do have that responsibility, even though he/she cannot write orders and are assumed to be responsible for carrying out orders written by physicians. Healthcare is a team endeavor. Nobody is infallible. In teaching hospitals the physicians caring for the patients are learning themselves. Everybody has the responsibility, when they have the skill, knowledge, and experience, to see that a patient receives the most optimal level of care. In the Healthcare – Pennsylvania State Education Association Patient Care – Limits of Accountability it states that: “The nurse will not be held legally accountable for errors made by the doctor – with one exception. If the reasonable nurse would recognize that an error is occurring, then the nurse caring for the patient has an obligation to notify the physician or his/her manager. Failure to do so may mean liability for the nurse. The doctor is held liable for his error; the nurse is held liable for failing to follow the standard of care and notifying appropriately. This is a violation of the nurse’s independent legal duty to exercise reasonable profession judgment to protect the patient (Patient Care: Limits of Accountability , 2015).
Following are some actual scenarios. If they involve cases the cases have settled or have gone through the trial process:
A gentleman presents to the Emergency Department with complaint of severe neck pain (10/10). He does not mention that he hit his head on a 2 x 4 3 days earlier and it is not documented, on the day he presented to the ED, that anyone pursued getting a history as to a possible injury that could have caused this acute onset neck pain. He was also noted to have a history of an aortic valve replacement and was on Coumadin. His presenting blood pressure was 192/95. He is given Dilaudid 1 mg IV and Toradol 60 mg IV. No further vital signs are taken prior to discharge. 90 minutes later he is so somnulent that he cannot sign the discharge instructions so a friend that came to take him home signs the paper. The resident writes for him to be discharged. 2 minutes after the discharge order is written a blood pressure of 210/66 is documented (the resident and attending physician in deposition state that they were not aware of his continued hypertension). He is discharged and the next morning his wife finds him unresponsive in bed with coffee ground material all over his chest. He is taken back to the ED by ambulance and is found to have a massive head bleed and a GI bleed. This case did settle. Did nursing have some liability in this case? I believe that they did. What are your thoughts? I believe that nursing should have questioned the discharge of someone that was so somnulent that they could not sign their name; that they should have questioned giving Toradol IV to a patient on Coumadin; and they should have notified the physician of the blood pressure they obtained prior to discharge.
A gentleman undergoes open heart bypass surgery and develops atrial fibrillation. He is discharged home and medical management is unsuccessful in converting his rhythm to normal sinus. He is seen in consult by a physician that performs atrial ablations. The written recommendation is that the patient undergo a TEE and then atrial ablation. He is then a short time later admitted to the hospital for the procedure. The atrial ablation is done but the TEE is not done. 12 hours later the gentleman suffers a massive stroke and within 24 hours is withdrawn from life support. Should nursing have known that it is a standard of care to perform a TEE prior to having an atrial ablation to rule out a left ventricular clot? The nursing personnel obviously would not have been privy to the consultant’s recommendation that a TEE be done. The physician in this case settled.
A young lady is in a terrible motor vehicle collision and has multiple internal organ injuries and fractures. Post stabilization in the operating room she is in the ICU, intubated and sedated. She has a peripheral IV that has propofol infusing. 4 hours prior to that peripheral IV being discontinued for swelling, there is one place in the 2200+ pages of medical records where the nurse documented swelling at the IV site. At 3:15 AM when he did discontinue the IV her hand was swollen and black. The physician became aware of the situation at 4 AM, which now had documented decreased pulses from prior assessments (they were palpable and now only present per Doppler). Then from 4 AM until this physician left at 10 AM the only thing done for this hand was elevating it. The day nurse documented at 11 AM the inability to get any pulses in that wrist but there is no documentation that a physician was notified. The patient went back to the OR at 1 PM to have her abdomen closed. At 5:15 PM a physician called in an ortho consult for her hand documenting that he had no idea how bad her hand looked. 45 minutes later she was in the OR undergoing fasciotomies to her left hand and forearm and has lasting decreased function of that arm. Did the nurse (forget that the IV site had swelling for 4 hours prior to being discontinued) have any responsibility for nothing being done for the young lady’s hand for hours? I believe that they did. When no action was being taken by the physician they first should have asked what his plan was for addressing this black, tight, swollen, cyanotic hand. If he did not have a plan then they had a duty to notify their manager or a nursing supervisor. When pulses were not obtainable the physician should have been notified (the fasciotomies might have been able to be performed when she went to the OR at 1 PM to have her abdomen closed). The hospital settled on behalf of the nursing staff in this case.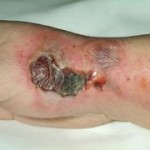
Yes doctors write orders and decide what the medical treatment plan is for the patient. That does not mean that the nurse should have no input. When nothing is being done in a situation that needs to be addressed the nurse has a duty to first have a conversation with the treating physician and then if the situation is not rectified they need to notify somebody above them that can help get the situation dealt with appropriately. Just because a doctor has the responsibility for writing orders does not mean that he is infallible. If the nurse has the knowledge and experience to know that an order can cause harm to a patient they need to speak up and address the situation with the physician. I always believed in these situations it was best to suggest a possible alternative to what was being ordered rather than simply saying I can’t give this medication or perform this treatment. I would comments as your thoughts or your own experiences.
Leave a Comment